Any skin changes can affect our self-confidence and social life; this may even be worse when large areas of our body are covered in reddish spots with white scales that can itch a lot, bleed and hurt. In addition to physical discomfort, a great deal of psychological distress can be caused to patients by the knowledge that people occasionally shy away from them because they are unsure if these scabs are the result of a nasty infectious skin disease. Although the word psoriasis originates from the Greek psoriasis, which means an “itch” or “scabies”, this inflammatory skin disease is certainly not contagious.
WHAT IS IT?
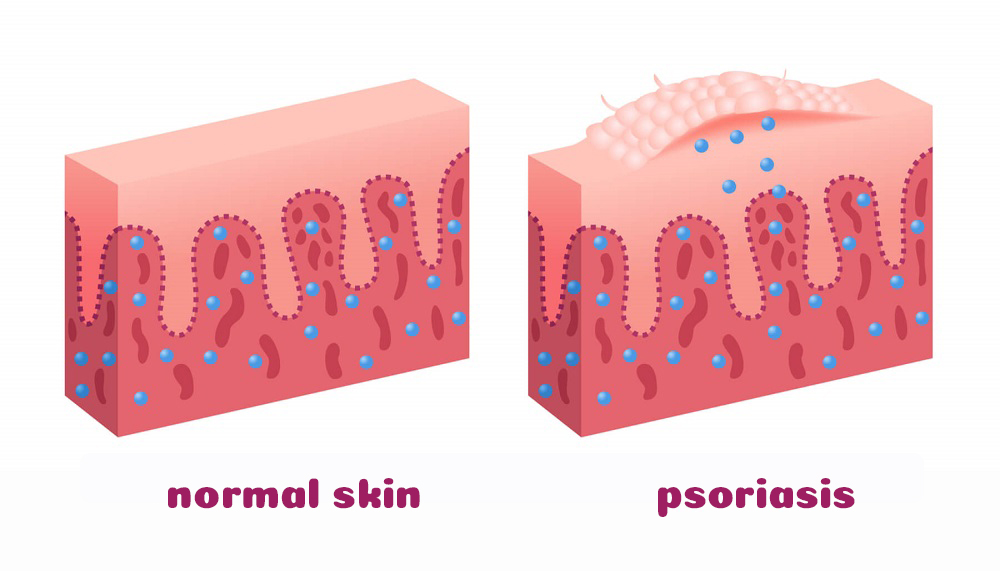
Psoriasis is a chronic inflammatory skin disease with a strong genetic predisposition and autoimmune pathogenic characteristics, which affects up to four per cent of the world’s population. It begins when keratinocytes, the cells of the epidermis – the outer layer of the skin, suddenly begin to multiply under the influence of T-lymphocytes, even up to six times more than normal. This creates pink scaly patches, especially in the area of the joints and folds of the skin, on the back, the genitals, feet and nails. Although science today is able to cure diseases that once afflicted millions, there is no specific cure for psoriasis and the same can be said for the exact medical explanation of the causes of psoriasis – there is none. What we know is that it is more common in patients under the age of 25, but it does not spare older people; it can suddenly strike women during menopause and people with impaired immunity; genetics plays a big role in its occurrence, it is more common in white people, slightly more common in women than in men, and in a large percentage of patients psoriasis is preceded by stress or psychological problems.
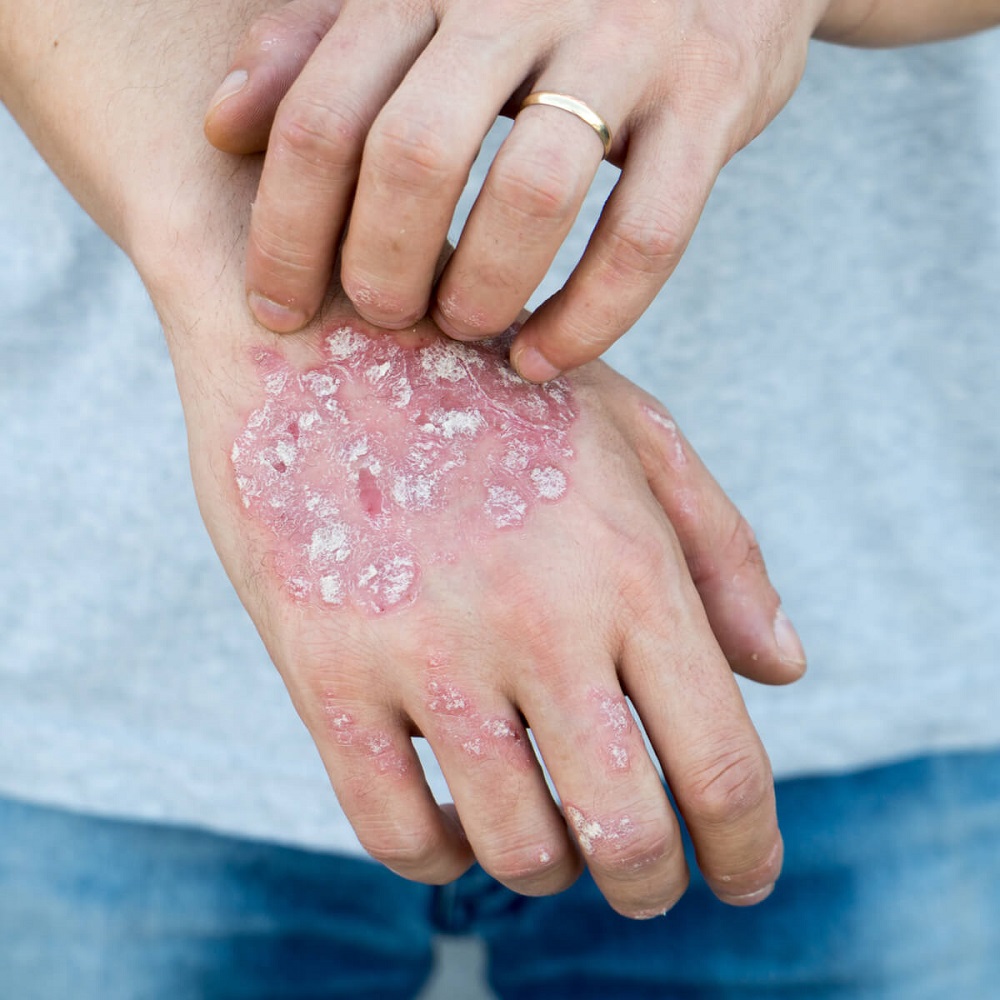
PSORIASIS: SYMPTOMS
The largest number of sufferers have a form called plaque psoriasis, named so because of the plaques, dry skin lesions covered in scales which itch and bleed easily when scratched. They come in waves, occasionally recede and reappear or even intensify. The changes on the skin decrease, sometimes disappear, but sometimes permanent marks remain. In some people, a psoriatic plaque can completely disappear and reappear after many years.
DOES PSORIASIS ITCH?
Yes: as its scientific name says, one of its symptoms is itching or pruritus which can be so strong that it interferes with falling to sleep or causes the patient to wake up during the night. Itching is particularly intense in inflammatory reactions. Some 20 percent of patients describe the itching as prickly, 15 percent of them as a burning sensation, and for 33 percent of patients the itching is extremely strong. As many as 75 percent of patients have an unbearable need to scratch until they bleed.
TYPES
Psoriasis has several subtypes; in most cases it is not life-threatening, but some of its forms, such as erythrodermic or pustular psoriasis, if neglected, can be fatal, because it may lead to heart failure or body overheating. This skin disease can also be combined with other diseases, such as psoriatic arthritis, an inflammatory disease of the joints in which antibodies are not produced and which is manifested by swelling and deformities of the joints. In addition to skin changes, psoriasis can distort and destroy nails or cause conjunctivitis, diabetes and depression. The diagnosis of psoriasis is established based on the appearance, location of the skin changes and severity of the disease.
There are several forms of psoriasis:
- In about 90 percent of cases psoriasis is manifested by classic symptoms and plaques covering the torso, the elbows, knees or the scalp. This is the so-called plaque psoriasis or psoriasis vulgaris.
- Inverse psoriasis occurs in skin folds, areas that are subject to friction, such as the glutes, armpits or the genital area and appears as smooth red psoriatic lesions.
- Guttate psoriasis, small drop-shaped sores, usually affects children and adolescents and is often triggered by streptococcal infections of the tonsils. Unfortunately, a third of these patients will develop plaque psoriasis later in life.
- Pustular psoriasis is manifested by the appearance of purulent nodules, most often on the hands and feet, including the nails, and is often very progressive.
- Erythrodermic psoriasis affects the whole body and can cause serious conditions because it impairs the body’s ability to regulate body temperature.
Scalp psoriasis is a common skin disorder, and clinical signs include reddish scaly patches on the scalp that can spread to the forehead, neck or around the ears. About half of all psoriasis patients have scalp psoriasis. In addition to itching, it also causes flaking of the skin that resembles dandruff, drying of the scalp and hair loss.
Psoriasis on the hands and feet is also common and is medically known as palmoplantar psoriasis. About 40 percent of patients with plaque psoriasis suffer from it. On the hands and feet it often affects the nails, especially the nail root, causing them to break, thicken or change colour; it can also cause the nail to separate from the nail bed. Nail psoriasis is often accompanied by fungal diseases.
In addition to arthritis, this unpleasant skin disease often increases the likelihood of developing other disorders, such as type 2 diabetes, cardiovascular disease and inflammatory bowel disease. It is not known whether psoriasis triggers these associated diseases or just accompanies them.

CREAM FOR PSORIASIS
It is interesting to know that Eskimos do not suffer from psoriasis, which may be related to the fact that essential fatty acids help in the treatment of the disease. In addition to the therapy we receive from dermatologists, sufferers find sea water very beneficial, as well as careful exposure to sunlight, which is why this disease usually subsides in the summer and intensifies during colder days. It is important to react to the emergence of the first symptoms of the disease in order to prevent its spread and complications.
Psoriasis can also be fought with good nutrition – by avoiding fast food, artificial sugars and simple carbohydrates; spring and autumn body detox therapy is also recommended. This also helps to keep body weight under control, because one of the triggers of psoriasis can be obesity.
Corticosteroids are often used for the treatment; they act quickly but should not be used over a long period of time. That is why sufferers of this unpleasant disorder need a natural solution that relieves itching and peeling and promotes skin healing. Fortunately, that solution exists.
Devi skin regeneration balm is a completely natural herbal formula without corticosteroids, preservatives and artificial substances. Quality butters – of shea and cocoa, as well as oils of avocado, jojoba, marigold, wheat germ and evening primrose, stimulate proper functioning of healthy skin and the healing of damaged skin. The real trump card in the composition of this beautiful balm when it comes to psoriasis is Chilean rose oil. Known as the ‘fruit of eternal youth’, the Chilean rose is a strong antioxidant that strengthens the skin’s immunity, has a cytotoxic effect and very efficiently stimulates the renewal of skin cells. Thus, the oil of this beneficial plant effectively prevents itching and flaking of the skin, helps epithelization of damaged parts and increases the skin’s elasticity by stimulating collagen production. It also enables healing – after the psoriatic plaque disappears, no visible marks will remain. Devi regeneration balm can be used indefinitely and is also ideal for daily skin care. Psoriasis is persistent, annoying and unpleasant, but Devi regeneration balm is even more persistent and firmly determined to contribute to our quality of life.

